Catholic Medical Quarterly Volume 64(2) May 2014
The spectrum of death:
an evolving culture in medicine
Eugene Breen
Editorial comment
It is important to note in the following article that ventilation is not always to be considered an ordinary form of treatment. And as Dr. Breen points out, Pope John Paul II’s declaration on euthanasia clearly states that to refuse extraordinary means “is not the equivalent of suicide; on the contrary it should be considered as an acceptance of the human condition, or a wish to avoid the application of a medical procedure disproportionate to the results that can be expected, or a desire not to impose excessive expense on the family or community”.
Introduction
 Death and dying are now big business. Visit a website for a
reputable undertaker and you will be dazzled by the amount of
money you can spend on gilt edge, platinum or plain yellow-pack
funeral arrangements! They read like a hall of fame and would be
comical if they weren’t so serious. Dying with dignity is the
catch call and is surely the way to go, but not before one’s
time. The timing of death is the nub of present controversy.
Campaigns for euthanasia, assisted suicide and pressures from
various care pathways to fast forward death, all lead toward a
worst case scenario of unlawful death becoming an option. The
innate human instinct is to preserve one’s life and that of
others. We are familiar with the idea of life becoming difficult
or even “unbearable”. Relatives or friends may also consider the
lives of their beloved as being “unbearable”. The result of this
type of thought process is: Why continue to suffer? Why
prolong the agony? This reasoning gives rise to death as an
option in all its dimensions, be it self harm, euthanasia,
assisted suicide, murder, etc. Ultimately, death becomes
acceptable as a real possibility, even a treatment, for
difficult situations be they medical, social or financial.
Death and dying are now big business. Visit a website for a
reputable undertaker and you will be dazzled by the amount of
money you can spend on gilt edge, platinum or plain yellow-pack
funeral arrangements! They read like a hall of fame and would be
comical if they weren’t so serious. Dying with dignity is the
catch call and is surely the way to go, but not before one’s
time. The timing of death is the nub of present controversy.
Campaigns for euthanasia, assisted suicide and pressures from
various care pathways to fast forward death, all lead toward a
worst case scenario of unlawful death becoming an option. The
innate human instinct is to preserve one’s life and that of
others. We are familiar with the idea of life becoming difficult
or even “unbearable”. Relatives or friends may also consider the
lives of their beloved as being “unbearable”. The result of this
type of thought process is: Why continue to suffer? Why
prolong the agony? This reasoning gives rise to death as an
option in all its dimensions, be it self harm, euthanasia,
assisted suicide, murder, etc. Ultimately, death becomes
acceptable as a real possibility, even a treatment, for
difficult situations be they medical, social or financial.
Background
In most societies life has more than just a material status. People have meaning and purpose in their lives, they have goals to achieve, and work and relationships to develop and enjoy. Many believe in God or a higher power and hope and yearn for a life hereafter. Millions, even billions of people live their lives according to the tenets of a religion or world view. This sometimes makes suffering understandable and equips people to endure illness and adversity. Life becomes worth living even in adversity.
The focus on end of life care ranging from excellent palliative care to euthanasia is an area of increasingly divergent concern. Bias is a powerful influence on clarity, and free/objective decision making, and end of life care is wide open to bias. These powerful influences include:
- Why continue the suffering when it has no meaning or sense?
- The suffering is disproportionate to the result of the treatment.
- The treatment is futile and onerous.
- The cost of ongoing treatment and demands on the work force and stretched budgets is enormous.
- The relatives find it all too stressful and don’t want to see their beloved suffer.
- The person is in a persistent vegetative state and “their quality of life is zero” and they would never have wanted this to be happening.
- For a person in a minimally conscious or vegetative state who cannot communicate, it could occur that the family wish for supportive care to end.
These and other combinations of concern may weigh heavily on health professionals pushing them towards hastening death. There may also be disagreement amongst the caring team and also among the relatives. For example what may constitute excessive care or unnecessary treatment could be theoretically based on:
- The suffering of the patient.
- The patient's wishes, either expressed now or in an advance directive, or what relatives know they would want.
- The suffering of the family, who do not want the beloved to suffer anymore.
- The cost on relatives or the state…..can this ongoing treatment be afforded?
Right to life
 To counterbalance these considerations one looks at the
patient’s right to life and the respect and value human life has
itself. Life, no matter what the quality, is human life, and as
such attracts all the protection of the law and all the human
rights of any other person. Most countries recognise the
inviolability of life once born and outlaw any unlawful killing
including euthanasia or assisted suicide. This is based on the
equality of all life and also to safeguard against abuse of
vulnerable people, sick people and dependent people. It elevates
the esteem with which life is held and respected and transmits a
reverence for all human life of whatever health. The
commandment “thou shalt not kill” further strengthens this
status in Christian countries. When life is not respected and
valued even at its most vulnerable level, there follows a
cheapening of the seen value of life for everyone. Murder,
suicide, abortion, and other acts become common. It has a
detrimental effect on society which becomes less safe and more
violent. This is seen in statistics of countries that are life
respecting like Ireland where the murder rate is low and
abortion illegal, and offences against the person much less than
in more “liberal” countries such as USA or UK.
To counterbalance these considerations one looks at the
patient’s right to life and the respect and value human life has
itself. Life, no matter what the quality, is human life, and as
such attracts all the protection of the law and all the human
rights of any other person. Most countries recognise the
inviolability of life once born and outlaw any unlawful killing
including euthanasia or assisted suicide. This is based on the
equality of all life and also to safeguard against abuse of
vulnerable people, sick people and dependent people. It elevates
the esteem with which life is held and respected and transmits a
reverence for all human life of whatever health. The
commandment “thou shalt not kill” further strengthens this
status in Christian countries. When life is not respected and
valued even at its most vulnerable level, there follows a
cheapening of the seen value of life for everyone. Murder,
suicide, abortion, and other acts become common. It has a
detrimental effect on society which becomes less safe and more
violent. This is seen in statistics of countries that are life
respecting like Ireland where the murder rate is low and
abortion illegal, and offences against the person much less than
in more “liberal” countries such as USA or UK.
The slippery slope idea is well founded and based on epidemiological patterns of human behaviour. When a population drinks more alcohol the prevalence of alcoholism and abusive use escalates. When substance abuse becomes common it develops into a part of “normal” growing up with awful consequences. The contrary also occurs. When there is widespread voluntary work, charitable work and good neighbourhood behaviour and widespread practice of religion the prevalence of violence drops. Thus to treat the hard cases of terminal suffering purely in isolation is not correct. The actions of any member of society impact on the rest of society and any law must take into account the greater good of society in general. It is well established in law that there are higher rights (of society as opposed to one individual) that trump those of individuals at times to safeguard the good of the community.
Faceoff between pragmatism and good palliation
The stage is set then between pragmatism (cost, bed usage, manpower use, and suffering) and human dignity (meaning of life, good of society, human right to life, religious belief) and also taking into account the wishes of the person. People kill themselves. This does not mean it is right and nowhere is it a human right. It has the effect of lowering the bar for others (others begin to consider suicide as an option). People need safeguards and protection, especially when going through a difficult time. Making death a treatment option is absolutely contrary to the right to life which the state has a duty to preserve and protect. “Mercy killing”, euthanasia in all its guises, and quality control of newborn or unborn, are all an assault on the right to life. These practices make it more difficult for vulnerable people to struggle on with what may be a difficult life experience. This is based on sound anthropology since even health is relative: the wealthier are healthier, and the poor even though they have enough money are less physically and mentally well. This is because they compare themselves with better off folk and also because they are less educated. “Keeping up with the Jones”, peer pressure, competitiveness, societal pressure, stigma, taboo and many other societal characteristics all point to the relative effect that society has on individual human behaviour and vice versa. Switching off a ventilator in the quiet of a private intensive care unit when the patient is not irrevocably dead or at death's door in Dublin sends ripples across Ireland. Hidden or not, it is not hidden because free human actions impact on society and others by their very nature. Shakespeare said through the mouth of Mark Antony in Julius Caesar: “the evil that men do lives after them; the good is oft interred with their bones.” It is beyond the scope or competency of this article to demonstrate the societal impact of a human act, hidden or not, but there is sufficient practical evidence to well prove that one person's actions influence others. In the case of making death easy to consider as a real option, and of making it accessible, this holds true as seen with: restricted abortion becomes abortion on demand; restricted euthanasia if not euthanasia on demand as of yet, certainly undermines elderly confidence; lowering the stigma of suicide sees the figures rise and copy-cat suicides arise; one mass school shooting engenders others, etc.
ITU scenario
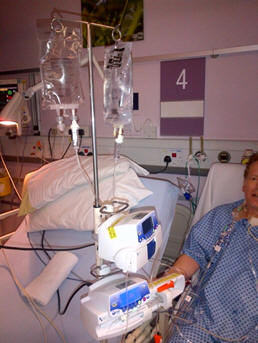
James is comatose and has a poor
prognosis. He is not expected to live and if he does he will
almost certainly require nursing care. Keeping the
ventilator working, it is not overly distressing.
Key
questions arise
- May you switch off the respirator and when?
- May you withhold fluid or nutrition or both?
- What does overburdensome mean?
- What does futile treatment mean?
- Is cost a consideration?
- Does prognosis influence what is done?
Taking these societal considerations into account what is right for this individual here and now in Intensive Care?
When in ITU is it too much, unnecessary and overzealous to treat a comatose or poor prognosis patient aggressively? May you switch off the respirator and when? May you withhold fluid or nutrition or both? What does overburdensome mean? What does futile treatment mean? Is cost a consideration? Prognosis is of significant importance, since once it is good or at least hopeful, every effort is exerted to help the person recover. When the prognosis is poor should pragmatic factors count? Let’s say switch off the ventilator and they die and keep it on and they live indefinitely in a minimally conscious state? Keeping the ventilator working, since it is not overly distressing and is relatively ordinary treatment, seems ethically sound since it respects the life of the patient and home ventilation is accepted practice in many countries. This does not mean that ventilation is always acceptable. There are various scenarios when ventilation may be refused, or not offered, because it is an extraordinary intervention in the circumstances, such as a poor prognosis elderly patient with pneumonia. Other similar poor prognosis cases also apply.
The present criteria according to accepted ethical guidelines are:
- Hydration and nutrition should always be administered provided they are not harmful, futile or over burdensome.
- Basic nursing care should always be attended to.
- To directly kill someone is a criminal offence.
- Ventilation and other life supporting treatments should be used to support life and comfort the patient.
- Antibiotics and other agents should be used when a medical gain is reasonably expected and not just used to prolong a dying process.
- Financial and resource elements are usually not an issue in the developed world.
Quality control or the quality of a life is not really the key issue. The job of the health professional is to serve life and not to determine if it meets some quality criteria. The new possibilities of life-prolonging treatments such as keeping babies of 24 weeks alive, elderly or terminally ill alive with intensive care input, and the seriously brain damaged or vegetative state people alive, raise questions. Do we have to do this? Just because we have the technology is it morally necessary? If we switch off now we have closure, the bed is free and the family are happy. The criterion of respecting life of whatever quality with usual medical means as outlined above means that even these fragile broken lives receive basic standard care.
The role of money, resources and extraordinary means
Alternatively one could say: “the nursing homes are filling up and costing a fortune, why not withhold expensive or not really necessary medications and not treat infections, and therefore cut costs?” This utilitarian approach is counter the duty to preserve life when one can, and could be seen as a slow track euthanasia based on utilitarian reasons. Some cancer drugs and operations are very expensive and as the tabloids say “Ellie won’t live unless she has the transplant and we are asking for donations etc.” This is a resource issue. Ellie needs the operation and hasn’t the money and will die unless operated on. Money here is the determinant and fair distribution of resources doesn’t reach as far as getting her covered, so her right to life is financially determined (provided the treatment has a reasonable chance of success). Money therefore does enter the equation at some level. However, fast forwarding death by withholding usual treatments in nursing homes is completely different. The concept of extraordinary means of prolonging life or treating illness could be invoked in Ellie's case (i.e. she is not morally obliged to undergo the treatment since it is “extraordinary” but can do so if she wants and can afford it), but certainly not in the case of the many elderly and ICU patients who just require basic routine care. The Vatican document on euthanasia by Pope John Paul II from 1980 clearly states that to refuse extraordinary means “is not the equivalent of suicide; on the contrary it should be considered as an acceptance of the human condition, or a wish to avoid the application of a medical procedure disproportionate to the results that can be expected, or a desire not to impose excessive expense on the family or community.”
To refuse extraordinary means “is not the equivalent of
suicide; on the contrary it should be considered as an
acceptance of the human condition, or a wish to avoid the
application of a medical procedure disproportionate to the
results that can be expected, or a desire not to impose
excessive expense on the family or community.”
Vatican
Declaration on Euthanasia
Concluding remarks
 The obligation to preserve, serve and protect life at all
stages with ordinary medical means (i.e. not necessarily having
to use extraordinary means that are not usually used) which are
the norm of the society, is the duty of the health care
professional. It is also the right of a patient to receive this
ordinary care. This may mean being on maintenance ventilation,
25 years in persistent vegetative state, PEG fed or totally
nurse dependent 35 years. No one can determine a life worth
living, not even the person themselves, since life is a
fundamental human gift which is beyond the individual person’s
decision to end prematurely, and which has societal value and
protection. On the other hand where treatments are futile or
ineffective it would be wrong to provide them.
The obligation to preserve, serve and protect life at all
stages with ordinary medical means (i.e. not necessarily having
to use extraordinary means that are not usually used) which are
the norm of the society, is the duty of the health care
professional. It is also the right of a patient to receive this
ordinary care. This may mean being on maintenance ventilation,
25 years in persistent vegetative state, PEG fed or totally
nurse dependent 35 years. No one can determine a life worth
living, not even the person themselves, since life is a
fundamental human gift which is beyond the individual person’s
decision to end prematurely, and which has societal value and
protection. On the other hand where treatments are futile or
ineffective it would be wrong to provide them.
